How Interdisciplinary Medicine helps to Reduce overall Healthcare Costs and How to Implement it
Dr. Wulf-Peter Brockmann, Founder and Radiation Therapist, Institut OncoLight
Willi Stappert, Founder & CEO, Verunion GmbH
Interdisciplinary medicine is an approach to healthcare that involves collaboration between different medical specialties. It has been shown to have several benefits, including improved patient outcomes, and reduced overall healthcare costs. This article discusses how interdisciplinary medicine can help to reduce overall health costs and how interdisciplinary groups can be build based on formerly independent practices and clinics.

Trends like ageing population on the one hand and rising public debt on the other put pressure on societies to reduce overall healthcare costs all over the world.
Governments in different countries try to keep costs under control by more or less the same measures even though with different weights on each of them. In general, these are:
• Encouraging preventative care
• Increasing price transparency
• Reducing administrative costs
• Encouraging the use of generic drugs
• Promoting telemedicine
• Value-based care
• Medicaid and Medicare reform
• Increasing competition among healthcare providers
As with any regulatory interference, all these efforts have their undeniable merits but exhibit destructive elements as well, if driven too far.
In the private sector different players promise to reduce costs by all sorts of new products and services in digitalization, high-tech diagnostics, etc. Only time will tell, what of these “innovations” actually add value and what is pure marketing/hype.
Another, more organizational, concept to reduce costs and improve outcomes for patients that has been around for years is interdisciplinary medicine on which we focus in this article.
Effects of interdisciplinary medicine in general
Interdisciplinary medicine, also known as team-based care, is a growing trend in healthcare that emphasizes collaboration between different medical specialties. This approach is designed to provide comprehensive, patient-centered care by addressing multiple aspects of a patient's health. Interdisciplinary medicine has been shown to have several benefits, including improved patient outcomes, increased patient satisfaction, and reduced overall healthcare costs.
In general, interdisciplinary medicine can help to reduce overall health costs by improving the coordination of care and reducing the need for duplicate or unnecessary tests and procedures. This is because interdisciplinary teams are able to share information and collaborate on treatment plans, which can lead to more efficient and effective care. Additionally, interdisciplinary teams are able to address multiple aspects of a patient's health, which can lead to better management of chronic conditions and fewer complications. Studies have shown that interdisciplinary teams can result in a reduction in hospitalizations and emergency department visits, as well as a decrease in overall healthcare costs. It is important to integrate accompanying socio-medical activities and medical professions such as physiotherapy in order to shorten inpatient stays. This integration must be initiated directly by the hospital, i.e., by the hospital staff, in order to shorten, for example, orthopedic hospital stays, on the one hand through the exact timing of pre-operative diagnostics and sufficiently long physiotherapeutic exercises, and on the other hand, post-operatively through the scheduling of post-operative rehabilitative measures, as has worked so well in the Netherlands for years.
Examples & applications
It is known that interdisciplinary care is associated with lower costs and fewer hospital readmissions for older adults with complex medical needs. Another primary way in which interdisciplinary medicine can help to reduce overall health costs is by preventing the development of chronic conditions. Chronic diseases, such as diabetes and heart disease, are responsible for a significant portion of healthcare costs in many modern societies. By addressing risk factors and promoting healthy behaviors, interdisciplinary teams can help to prevent the development of these conditions and reduce the need for expensive treatments.
Also, interdisciplinary medicine is known to reduce overall health costs is by improving the coordination of care. In traditional healthcare systems, patients may see multiple healthcare professionals for different conditions, leading to a lack of coordination and communication. This can result in duplicative tests and treatments, leading to increased costs. Interdisciplinary teams, on the other hand, work together to provide coordinated care and communicate effectively with one another, which can help to avoid these issues.
In the case of cancer treatment, interdisciplinary medicine can play an especially important role in reducing costs. Cancer treatment can be complex and costly, and often requires the expertise of multiple specialists. Interdisciplinary teams can help to ensure that patients receive the most appropriate and effective treatment, which can reduce the need for repeated or unnecessary treatments. Additionally, interdisciplinary teams can help to manage the side effects of treatment and provide supportive care, which can improve patient outcomes and reduce costs associated with complications or hospitalizations. It must be remembered that it is not always the most expensive oncological drugs that achieve the best effect, but possibly cytostatic drugs that have been used successfully for decades.
The same applies to oncological treatment with the aid of medical equipment. In each individual case, it is necessary to cost-critically examine when the most expensive maximum-dose radiation therapies come into question, and when series with radiofrequency treatments in combination with further, also chemotherapeutic treatments in low doses, can ultimately be used to achieve the same goal. A typical example from Germany would be:

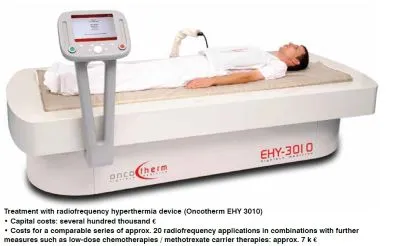
Interdisciplinary medicine can also help to reduce overall health costs in the case of cancer treatment. Cancer is one of the most costly diseases to treat and manage, and the cost of cancer care continues to rise. An interdisciplinary team can improve the coordination of care for cancer patients, which can help to reduce the costs of treatment and improve patient outcomes.
However, interdisciplinary teamwork using different therapeutic and diagnostic methods must not give physicians in an economically particularly lucrative area a financial advantage over other colleagues in their team.
Another practical example is integrative medicine, which combines conventional and complementary approaches to healthcare, can also contribute to cost savings in cancer treatment. For example, integrative medicine can include the use of complementary therapies such as acupuncture, massage, and mind-body practices. These therapies can help to reduce symptoms and improve quality of life for cancer patients, which can reduce the need for additional medical treatments and medications. Additionally, integrative medicine can include the use of dietary and lifestyle changes, which can help to prevent and manage chronic conditions and reduce overall healthcare costs.
Obstacles and possible solutions by private healthcare providers
The whole idea of interdisciplinary medicine has been there for decades now. Its widespread implementation, however, faces several obstacles. These include a lack of communication and coordination among different healthcare professionals, a lack of training in interdisciplinary care, and a lack of reimbursement for interdisciplinary services. The latter may or may not be ever resolved, as it would require innovative thinking on behalf of politicians and their will to reconfigure regulation. The industry can, however, make steps to resolve other obstacles themselves.
One strategy would be to build topic-specific groups for instance in the field of cancer treatments using a combination of mergers & acquisitions of clinics and practices as well as targeted greenfield investments. Such group can include practices / clinics in the field of:
• Diagnostics (radiology, laboratories, pathology)
• (Pharmaco-)Oncology
• Radio-oncology
• Nuclear medicine including diagnostics and therapies
• Treatments from alternative medicine by electromagnetic fields and hyperthermia
Such groups should then be led by one overall management and governance at the strategic level. This management should take the following steps to develop it into an effective specialized group:
Promote communication and collaboration among its healthcare professionals through the use of electronic medical records, interdisciplinary rounds, and regular meetings.
1. Provide training and education in interdisciplinary care so that healthcare professionals develop the skills and knowledge necessary to effectively collaborate with their colleagues.
2. Develop “internal” reimbursement models that support interdisciplinary care. This would ensure that formerly independent practices/clinics are financially incentivized to work together to provide comprehensive care for patients.
3. Use telemedicine and other forms of remote communication so that healthcare professionals from geographic locations can collaborate and share information effectively.
4. Complement the often too generalists service portfolio of the formerly independent practices (e.g., radiology, laboratories) with more specialized expertise within the group’s strategic framework.
5. Support interdisciplinary research to improve understanding of disease and advance new treatment strategies that can be shared within the group to improve patient outcomes and to enhance the group’s profile.
6. Annual compulsory periods for collaboration or on-site observation in the other specialties for their better understanding (e.g., PET-CT diagnostics, expansion of the use of laboratory tumor markers)
7. Preventing the intrusion of particular external interests into individual areas of expertise within a team.
8. Prevention of isolated special oncological diagnostic and therapy centers that create their own guidelines and pay so much attention to their own profitability that there is a danger that inexpensive but successful alternatives outside these centers will hardly be considered as off-label use.
It is important to summarize that the obstacles to interdisciplinary medicine are not technological ones. They are partly regulatory but first and foremost organizational.
So far, strategic or private equity consolidators in the healthcare sector focused almost entirely on “mono-cultural” approaches: buying up smaller players (practices or clinics) in the same discipline as dentistry, radiology, ophthalmology and create big player. Most of the time, this buy & build projects are not followed by an appropriate integration. Also, true synergies between the acquired targets in such a mono-cultural groups are oftentimes rather limited. But almost never do these kinds of consolidations lead to any significant added value for patients. The consolidators love these projects because the value of a bigger group is disproportionately larger than the sum of the valuations of its separate elements. These groups can be then listed publicly or resold with handsome profits.
If the concept of interdisciplinary medicine is to be taken seriously, it seems worthwhile not only to concentrate on the above-mentioned specialist areas, but also to economically combine interdisciplinary oncological therapists together with their essential environment in the same way, so that the result is an overall oncological network that is as comprehensive as possible, in which no physician outperforms another of the same hierarchy financially and thus also does not allow overvaluation of individual areas.
The biggest problem of such cost containment, however, is the pharmaceutical industry, which up to now in Germany has been able to dictate its prices practically without resistance and even forces prices up to 50% higher when it discontinues common drugs under various arguments.
In Germany in recent years, a few consolidators started to acquire practices from different disciplines. However, if there is an actual strategy behind it, it is to get big fast for the same reasons as above and/or secure sales synergies (for instance between orthopedics and radiologists) which is a legal grey zone area. These approaches are not patient-centric either and are purely commercial.
Building a true interdisciplinary group and realizing all its intended benefits is beyond the comfort zones and not in line with incentive structures of most consolidators who more often than not are led by ex-investment bankers or ex-management consultant. It is ultimately down to strong teams of charismatic entrepreneurs and medical professionals to put the idea into reality.




